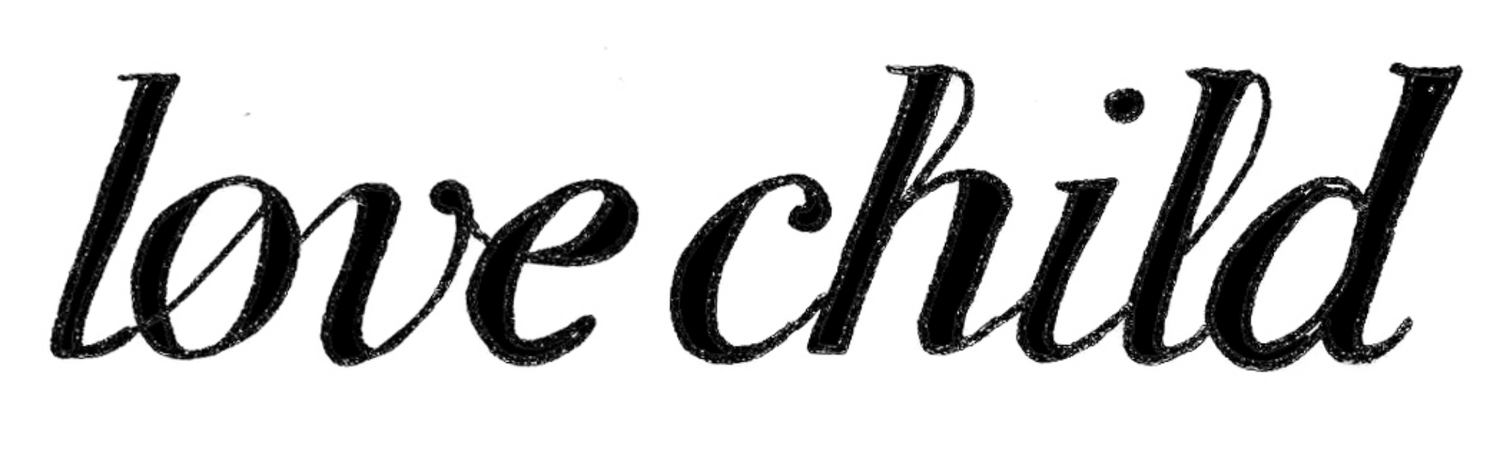They should give you a due-range, rather than a due-date.
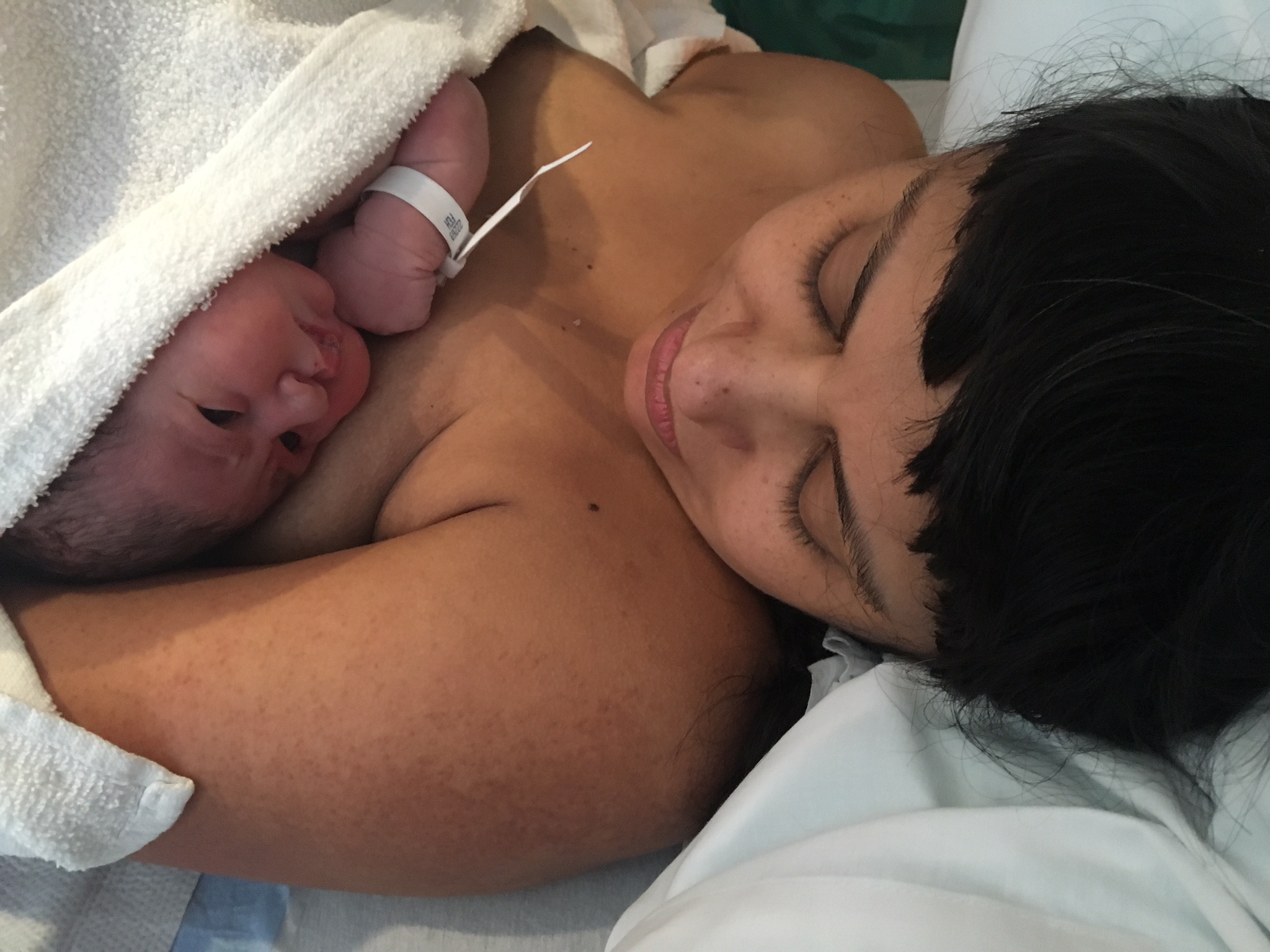
When October 5th came and went with no contractions, no sign of baby, and a fully nested-and-back-again apartment, I was beginning to think she’d never arrive. I’d already packed up my desk and begun staying home from work in anticipation of my little girl’s arrival. I was excited to meet her. And more than a little bit impatient.
Eight uneventful days after that uneventful day, I took a nap. In any other context, this was a marker of a good day. And that nap followed a vigorous prenatal massage, so as any sleep-deprived new parent will attest, this was indeed a Good Day.
My post-massage-and-nap glow was cut short when something occurred to me: I couldn’t remember when I’d last felt baby kick. I’d felt something at breakfast, again during the morning massage. But then – nothing. And it was now close to 5pm.
They say that you, as the mum, get to know what’s normal for your baby in terms of movement. And you do. It’s important to be aware of any deviations from the norm. My doctor had said previously that “moms often leave it too late.” On that chilling line, I followed up no further.
My baby liked to move though – pretty much nonstop tumbling and kicking - with two exceptions.
The first one was on a business trip I’d taken to San Francisco. My baby was eerily still for a couple of hours, and unresponsive to juice (the sugar is supposed to wake them up). My doctor, who’s usually pretty laid back, instructed me to go to a hospital with a labour-and-delivery unit right away. Embarrassingly, and magnificently, the baby kicked as they were checking me in to the hospital (which, as an aside, took way too long given how urgent the matter could have been).
All was well, and I cried a tear (or a hundred) of relief. My husband was on the point of driving from NYC to San Francisco without stopping, so the good news was particularly welcome.
The second time was on this day, 8 days after my due date, post massage and post nap.
I tried to remain calm.
At this point, it’s worth noting that I’d recently read a story from a woman who shared my due-date on TheBump.com. She had tragically lost her baby around week 40. After the baby stopped kicking, which she hadn’t really noticed.
So, you could say that my state of mind was quite dark.
Guilt flooded my body. What kind of selfish, spoiled person – lounging around her home on a work day following an indulgent massage - takes a nap and forgets to count kicks? A terrible mother, I told myself. (No one really tells you about the wildly irrational guilt involved in this kind of thing. But it’s not unusual.)
Anyway, I called my doctor after only a minute’s hesitation (“Stop being so British and polite all the time,” I could practically here my husband saying – though I was sparing him the news until I’d spoken to the obstetrician).
“Come to the hospital right away,” she said.
I could see that my husband was parking the car after work (thanks, iPhones), so I waited to tell him in person a few moments later. In the meantime, I texted my doula.
No reply.
My husband arrived. He snapped into action right away, trying to reassure me and be practical, but clearly worried sick himself. This isn’t the ending either of us had pictured.
He reached for the overnight bag I had packed so many weeks before – but I stopped him. I pictured myself grieving over my lost baby (getting a little ahead of myself to be sure) and unable to face the task of unpacking those unworn baby clothes at the hospital. In that surreal moment, it felt like taking the bag with us would jinx everything. Apparently this intense and scary episode brought out a superstitious side of me.
We headed outside to hail a cab. The cab driver, unlike every other New York taxi driver I’d encountered in my 15 years of visiting and residing in the city, stopped for every amber light and yielded to every other car, bus, and cyclist on the road.
But we got there. We were checked in quickly and they hooked me up to various machines. I had to click a little button every time I felt a kick, which mercifully didn’t take long. Baby was doing OK.
At this point, my doctor appeared. “We’re not sending you home tonight. You’re 41.5 weeks. It’s time.”
I’d had my heart set on a natural delivery, with minimal interventions. No induction, no epidural. That’s why I had a doula. (Who was still MIA and failing to respond to texts, by the way. This was out of character for her.)
They hooked me up to a Pitocin drip. Pitocin is synthetic oxytocin, and it’s one of a few ways hospitals try to induce labor. I was apparently already having mild contractions, but I couldn’t feel them in all the excitement. They picked up to a noticeable level when they gave me a saline drip. In all the post-nap commotion, I’d neglected to hydrate.
So there I was in the delivery room, getting comfortable. My husband left to get the bag we’d packed, and to make sure our dog was looked after.
The room was large and had a TV, which the nurse switched on.
“I don’t really want too much Pitocin,” I said.
She answered, “Don’t worry – we start on a super low dose, and try to only increase it as your contractions grow.” This was cheering.
The TV was showing the Democratic presidential candidates’ debate, which felt so quotidian on what was an exceptional day for our little family.
At first, the sensation felt like menstrual cramps. The contractions grew, and came quicker. I was managing, but they were definitely getting more noticeable as the Pitocin dose was increaed.
My husband returned and I was delighted to see him. He’d brought our suitcase, a nursing pillow, and some contraband snacks to sustain us both.
My doula texted apologetically. Another client was in labor and she wouldn’t be able to join us. She encouraged me to call on her back-up doula. To do it over again, I would have. But already flustered and feeling as though a few things out of my control were happening, I didn’t want to introduce another variable – a doula I didn’t feel 100% comfortable with.
So my husband and I soldiered on alone. The gaps between nurse visits felt long, and we didn’t see a doctor all night (this is normal, apparently). Both of us being new to labor, we weren’t sure we were doing it right. We’d taken classes and read books, but no one had really prepared us for the hospital experience, replete with its long waits and rigid but apparent-only-when-broken rules.
Apparently we were doing something right, because the contractions were coming faster and with more force. I later learned that one of the main disadvantages of medically induced contractions over natural ones is that the latter are accompanied by endorphins, and therefore significantly more bearable than their synthetic counterparts.
Another quirk of induction is that you are likely to be constantly monitored (i.e., hooked up to various machines) so it’s harder to move around. And standing/gravity helps labor progress, so this felt a little bit handicapping. My husband mentioned this to the nurse – I refer you to my aforementioned “damn Britishness” and aversion to anything akin to “making a fuss” – and she helped me out of the bed so I could stand up and try to get more comfortable. Standing helped – I felt like I was actually doing something to help the process along, versus just lying there.
The other wonderful part of this interaction was the news that “Other women on the ward have been dropping like flies for the epidural. You’re our hero.” Call it reverse schadenfreude, but this sustained me for another hour or so.
The pain continued to increase. At no point did I find myself emitting low, therapeutic moans like I’ve heard other women talk about. I was screaming and cursing and falling apart a little bit.
I was struggling with my breathing exercises for a maddeningly simple reason: I’m allergic to dust, which didn’t seem relevant in a hospital environment, but 100% was – the hospital’s birth center was under construction and my room neighbored the worksite. Had I known this, I’d have asked for an antihistamine hours prior. I got one eventually, other concerns overtook my respiratory issues.
It’s hard to describe the pain. I was in “back labour,” which I became convinced could make even a hardened terrorist speak under questioning. It felt like I was both outside my body and feeling pain more acutely than I’ve ever felt any sensation in my life. I’d crossed over from managing the pain to it managing me. In effect, I was fighting it – bracing hard for every coming contraction and feeling them at full force, with tears in my eyes.
As it was, eleven hours in, I started asking for an epidural. The nurse calmly explained that the anesthesiologist had just gone into surgery and would be at least an hour and would that be OK?
I not so calmly shouted “WELL WHAT CHOICE DO I HAVE!?”
Who was I?!
She returned much earlier than planned – anesthesiologist in tow. He worked quickly. We will never know the extent to which this might have been due to her having violently pulled him out of someone else’s operation to quiet down the woman who was screaming in room three.
I was still feeling the pain, but the sight of this man and his glorious cart of drugs sustained me as they prepped me for the procedure. My husband was given a surgical mask and told to look away. (Our childbirth educator mentioned that partners fainting was one of the main hazards of epidural delivery.) He was fine.
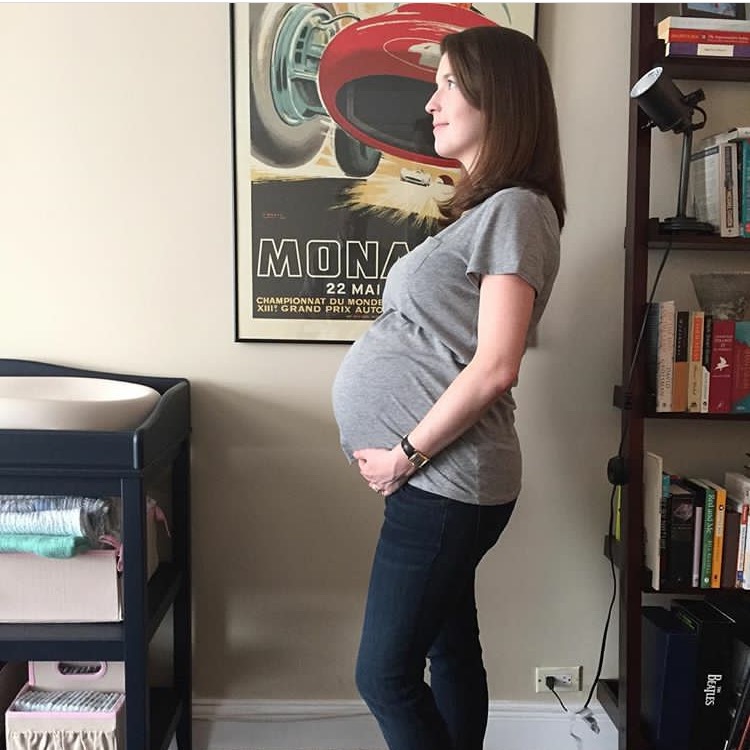
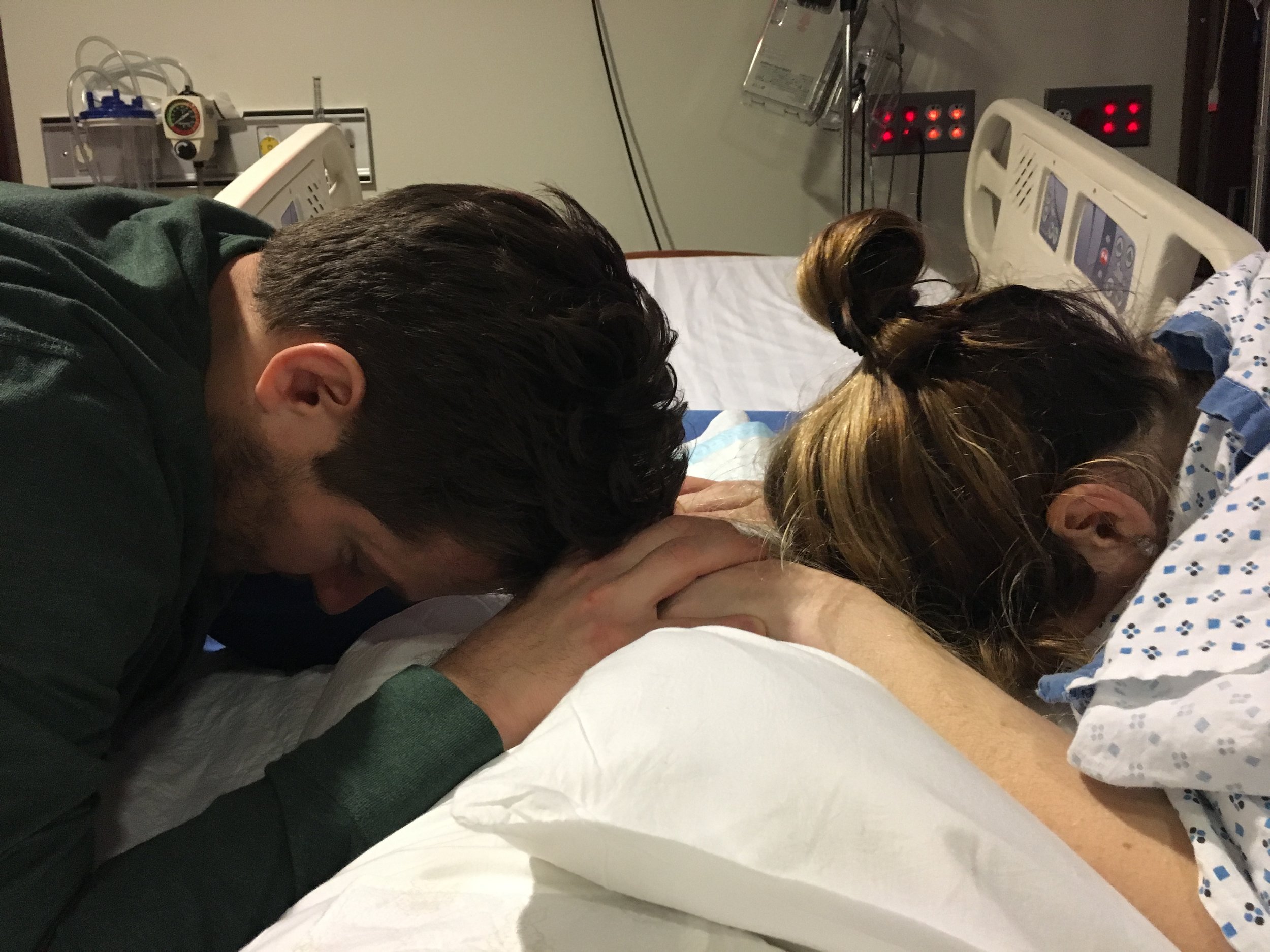
I perched on the edge of the bed and leaned towards the nurse while the anesthesiologist prepared the needle for my spine. I’d always had an aversion to the very idea of a needle near my spine, so that in itself attests to the pain I was feeling.
He did it. And the pain accompanying each contraction seemed to recede into gentle nothingness. The best thing about this? I could sleep! The second best? My husband could sleep! It was morning, and we’d essentially pulled an all-nighter in which one of us had run a marathon while the other had jogged alongside the other, worrying about the other’s health throughout. We’d earned a nap.
I woke a few hours later, feeling refreshed and ready to push.
They’d shown me a button to press which might as well have been labeled “MORE DRUGS”, but I didn’t use it. The initial dose was plenty, and began to wear off in time for the pushing. I was glad: I could feel a bit of pressure when I needed to push, but no pain.
It’s worth mentioning here that the morning crew wasn’t as competent as the overnight one. Doctor and nurse each had a trainee with them, and seemed more interested in showing their apprentice the ropes than providing my baby and me with medical care. Case in point: my husband had to ask for the nurses’ help each time I was ready to push because one was showing the other how to inventory the supply cupboards and neglecting to look at me or the monitors.
I heard the overnight nurse remind them to catheterize me so I could urinate at a particular time, but they forgot. A small error, but one with serious repercussions: baby’s heartrate was falling and it was only when they helped me empty my bladder that it picked up. They laughed at this. We did not.
Every time I pushed, my baby’s heartrate dropped again before picking up between contractions. This was stressful, and made worse when the doctor dropped by to simply say “Baby does not like your pushes” then left. Thanks for the vote of confidence, lady.
They gave me oxygen to use between pushes, and had me roll over to my left side in between each one as this helped baby’s heartrate recover. Again, my husband had to prompt me each time as the nurses were otherwise engaged.
After 1.5 hours of this, the doctor arrived to oversee the actual delivery. During a contraction, I thought I heard her say quietly, matter-of-factly, “Let’s cut now.” And it turns out I did, because I later learned they’d elected to give me an episiotomy.
Emergency medicine doesn’t always allow for explicit patient consent, but I only wish they had told me – if not asked me or my husband - at any point before, during, or after. But they didn’t. I never learned why it happened and how urgent the matter was, if at all. Simply but directly informing me of what they were doing to my body would have made the experience significantly easier to process after the fact.
Anyway, back to the pushing. They asked if I wanted to feel the baby’s head as she crowned. I surprised myself by saying yes. It was oddly cheering – a surreal reward for having made progress. The cord was wrapped around her head – they unwrapped it, and after pushing the head out, the rest of the labor felt quick.
Baby was born after 12 hours of labor and 2 of pushing. They put her on my chest and she latched fairly quickly. They had to clean her up and examine her, so I gave her to my husband after he cut the cord, and he took her to the other side of the room to be examined. I watched this process from my bed as I delivered the placenta and got stitched up.
Because of the epidural, I couldn’t feel my legs and therefore couldn’t stand up. I also learned that gravity has bearing on this: my leaning to the left during contractions meant my right leg regained feeling faster than the left. A funny sensation.
Despite the challenging night (and morning), I was happier than I’ve ever been.
The endorphins that eluded me during the night flooded my body. I was ecstatic. I was a mum to a beautiful daughter. And I’d do it all again – but perhaps a little differently.